When seniors take medications for pain, anxiety, or sleep, their bodies don’t process them the same way they did at 40. Their liver slows down. Their kidneys filter less. Their brain becomes more sensitive. This isn’t just a minor change-it’s a ticking risk. Every year, over 200,000 adverse events linked to sedatives and opioids happen in U.S. healthcare settings. Of those, 65% involve patients over 65. Many of these cases could have been avoided with better monitoring. The question isn’t whether to watch for signs of over-sedation-it’s how to do it right, before it’s too late.
Why Seniors Are at Higher Risk
A 75-year-old taking the same dose of morphine as a 30-year-old isn’t getting the same effect. Their body holds onto the drug longer. Studies show that between ages 20 and 80, liver metabolism drops by 30% to 50%. Kidney function declines by about 0.8 mL/min/1.73m² every year after 40. That means drugs build up. Even small doses can push someone into dangerous territory. Add in conditions like COPD, heart failure, or dementia, and the risk multiplies.Here’s the scary part: seniors often don’t show obvious signs of trouble until it’s critical. They might not groan, flail, or gasp. Instead, they go quiet. Their breathing slows. Their oxygen levels dip slowly. By the time their pulse oximeter alarms, it’s often too late. That’s why relying on one tool-like pulse oximetry alone-isn’t enough.
The Five Vital Signs to Watch
Monitoring a senior during sedation isn’t about checking one number. It’s about watching five things together, all the time.- Pulse Oximetry (SpO2): Keep oxygen saturation above 92%. Alarms should trigger at 90%. But here’s the catch: if a senior is on supplemental oxygen, their SpO2 can stay at 95% even while they’re dangerously under-breathing. Oxygen masks can hide the real problem.
- Respiratory Rate: Below 8 breaths per minute is a red flag. Normal is 12-20. If it drops to 6 or lower, stop the procedure. This is often the first sign of opioid-induced respiratory depression.
- End-Tidal CO2 (EtCO2) via Capnography: This measures carbon dioxide in exhaled breath. Normal range: 35-45 mmHg. A flat line or a sudden drop means no breathing-or not enough. Capnography detects apnea 92% of the time in seniors, while pulse oximetry misses it in 33% of cases when oxygen is being given.
- Heart Rate: Below 50 or above 100 beats per minute can signal distress. A slowing heart rate often follows slowed breathing. Don’t ignore it.
- Blood Pressure: Systolic pressure below 90 mmHg is a warning sign. Low BP can mean the body is shutting down from too much sedation.
These aren’t optional. The American Society of Anesthesiologists (ASA) says continuous monitoring of all five is the minimum standard for anyone over 65.
The Gold Standard: Multimodal Monitoring
Using just one monitor is like driving with only a speedometer. You need more. The best approach combines multiple tools into one system.The Integrated Pulmonary Index® (IPI) is one of the most reliable. It takes data from capnography, pulse oximetry, heart rate, and respiratory rate-and turns it into a single score from 1 to 10. A score below 7 means trouble. A 2021 study of 1,245 elderly patients found that IPI detected breathing problems an average of 12.7 minutes before oxygen levels dropped. That’s more than enough time to react.
Another powerful tool is Respiratory Volume Monitoring (RVM). It uses bioimpedance sensors to measure how much air moves in and out of the lungs. Unlike pulse oximetry, it doesn’t need oxygen to be present. In a 2019 study, RVM flagged hypoventilation 14.3 minutes before the pulse oximeter went off. But there’s a catch: it requires electrodes stuck to the chest, and older skin is fragile. In 22% of cases, the sensors don’t stick properly.
For sedation depth, use the Richmond Agitation-Sedation Scale (RASS). It scores consciousness from +4 (agitated) to -5 (unresponsive). A score of -2 means moderate sedation. -3 is deep. -4 or -5 is dangerous. Nurses trained in RASS can spot changes before vital signs crash. At Mayo Clinic, combining RASS with capnography cut oversedation events by 41% in patients over 75.

What Not to Do
Many mistakes come from old habits.- Don’t rely on intermittent checks. Checking every 5 minutes misses 78% of breathing events. Seniors can go from fine to unresponsive in under 3 minutes.
- Don’t trust pulse oximetry alone. A 2020 study in Gastrointestinal Endoscopy showed that 33% of seniors on oxygen had dangerous hypoventilation while their SpO2 stayed above 94%. Their lungs weren’t moving enough air-they were just breathing into an oxygen mask.
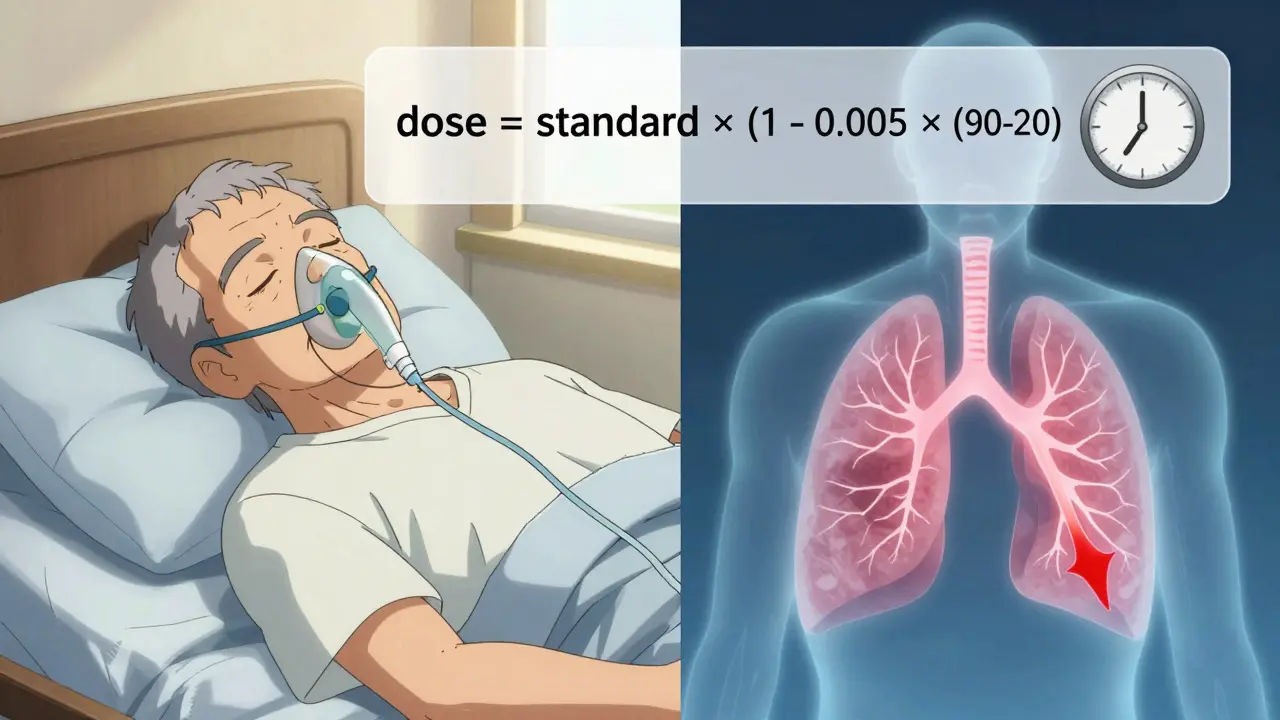
- Don’t use standard adult doses. A 2023 report found that 42% of facilities still give seniors the same opioid dose as younger adults. The fix? Use this simple formula: dose = standard dose × (1 - 0.005 × (age - 20)). For a 75-year-old, that’s about 27% less than the adult dose.
- Don’t ignore false alarms. Capnography has a 38% false alarm rate in seniors because their breathing is irregular. But ignoring alarms because they’re “always wrong” is dangerous. Look at the trend. Is the EtCO2 slowly rising? Is the respiratory rate dropping? Combine data.
Technology Helps-But People Save Lives
New tools are powerful. The FDA approved the Opioid Risk Monitoring System (ORMS) in 2023. It’s an IV pump that automatically pauses opioid delivery if the patient’s breathing drops below 8 breaths per minute. In a 2022 trial, it cut respiratory depression events by 58% in seniors.But technology can’t replace vigilance. A 2023 report from the National Commission for Quality Assurance found that 63% of oversedation cases happened because staff didn’t check on patients often enough. Another 29% involved misreading SpO2 numbers on oxygen.
Dr. Karen Posner, who helped write the 2016 APSF guidelines, says: “Capnography plus pulse oximetry is the minimum. But you still need a nurse watching, thinking, and responding.” In one case shared on Reddit, a nurse anesthetist saw an IPI score drop to 5.2 during a colonoscopy. The patient was 82. Oxygen levels were fine. But the IPI told the truth: breathing was failing. They stopped the procedure. Saved.
What to Do If You See Trouble
If you notice any of these signs:- Respiratory rate below 8
- EtCO2 below 30 or above 50
- SpO2 dropping despite oxygen
- RASS score of -4 or lower
- Heart rate below 50 or above 100
Act immediately:
- Stop giving sedatives or opioids.
- Give oxygen (but don’t rely on it to mask the problem).
- Stimulate the patient-talk loudly, shake gently.
- If no response, call for help and prepare for airway support.
- Consider naloxone (Narcan) if opioids are involved. But don’t wait for confirmation-act fast.
Delaying means death. In a 2021 incident at Massachusetts General Hospital, a 90-year-old died during a feeding tube placement because staff only checked oxygen every 10 minutes. The patient stopped breathing 7 minutes in. No one noticed until it was too late.
Training and Tools That Work
Most nurses need about 8 hours of training to use multimodal systems well. That includes:- Reading capnography waveforms-knowing what a “shark fin” pattern means (COPD) vs. a flat line (apnea)
- Using RASS consistently (inter-rater reliability is 0.87 when staff are trained)
- Applying age-based dosing formulas
- Choosing skin-friendly electrodes (hydrocolloid dressings reduce skin injury by 67%)
Facilities that train staff properly see big drops in incidents. The Joint Commission reports that 92% of U.S. hospitals now meet ASA monitoring standards, up from 67% in 2015. But outpatient centers lag. Only 42% use continuous monitoring. That’s where most seniors get sedated-for colonoscopies, dental work, minor procedures. This gap needs closing.
The Bottom Line
Monitoring seniors for over-sedation isn’t about fancy gadgets. It’s about combining smart tools with trained eyes and quick action. Capnography, pulse oximetry, RASS, and continuous vital sign tracking aren’t optional-they’re the bare minimum. Doses must be lowered. Checks must be constant. And someone must be watching, always.If you’re caring for an elderly loved one at home, talk to their doctor. Ask: “Are you using capnography? Are you adjusting doses for age? Are you checking breathing, not just oxygen?” If the answer is no, push for change. Lives depend on it.
What are the earliest signs of over-sedation in seniors?
The earliest signs are subtle: slower breathing (under 10 breaths per minute), slight drowsiness (RASS score of -1 or -2), and a drop in end-tidal CO2 (EtCO2) below 35 mmHg. Pulse oximetry may still look normal, especially if the senior is on oxygen. The key is watching trends, not single numbers. A steady drop in respiratory rate over 5 minutes is more dangerous than one low reading.
Can pulse oximetry alone detect opioid overdose in seniors?
No. Pulse oximetry measures oxygen in the blood, not breathing effort. Seniors on supplemental oxygen can maintain SpO2 above 94% even while their lungs are barely moving. A 2020 study found that 33% of seniors with dangerous hypoventilation had normal oxygen levels. Capnography, which measures carbon dioxide exhaled, detects breathing failure before oxygen drops. That’s why capnography is required by guidelines for patients over 65.
How much should opioid doses be reduced for seniors?
Use this formula: dose = standard adult dose × (1 - 0.005 × (age - 20)). For example, a 75-year-old should get about 27% less than the standard adult dose. A 90-year-old needs roughly 45% less. This accounts for slower metabolism and increased brain sensitivity. Many facilities still use adult doses, which is why overdoses are so common in this group.
Is capnography expensive or hard to use?
Capnography devices cost between $1,500 and $3,000, depending on features. Training takes about 3-4 hours for nurses to interpret waveforms reliably. The biggest barrier isn’t cost-it’s habit. Many clinics still use intermittent checks because they’re easier. But the data is clear: continuous capnography prevents 87% of respiratory arrests in seniors. The cost of one preventable death far outweighs the equipment.
What should I do if I suspect my elderly relative was over-sedated at a clinic?
Ask for the monitoring records: Were capnography, pulse oximetry, and respiratory rate tracked continuously? Was RASS or another sedation scale used? Was the dose adjusted for age? If the answer is no, request a review from the facility’s patient safety officer. Report it to your state’s health department. Many oversedation cases go unreported because families don’t know what to look for. Your question could prevent another tragedy.

